7:18 AM
Gabriel spent the night with his mom. Everything went well.
7:38 PM
Hold on tight, I have a lot to tell!
Summary of the discussion with the doctor:
Gabriel is in a serious but stable condition, as usual.
They took two X-rays today, as the first one wasn’t clear enough. According to him, there’s a slight improvement in some areas, but there’s still:
- atelectasis of the upper left lobe and lower right lobe,
- and a new phenomenon probably called pneumocele in the upper right
I asked why, just after the ECMO, his lungs seemed better, and why today they are more damaged. He explained that after bronchiolitis, there are two possible scenarios:
- either the lungs gradually recover,
- or it evolves into obliterative bronchiolitis, and unfortunately, this seems to be happening with Gabriel.
He told me they’re doing everything to prevent it from getting worse and to avoid his lungs being too damaged.
I also mentioned that during each physiotherapy session, Gabriel regurgitates what looks like bile, and I’m afraid it might cause infections. He replied that it wasn’t serious and that we shouldn’t worry about it… so there you have it…
Current treatment:
Azithromycin + corticosteroids + other antibiotics, still ongoing until Monday.
What’s planned next (if I understood correctly):
On Monday, they will take a sample from the trachea to check if the Stenotrophomonas maltophilia bacteria is still present.
- If it’s still there, another 15 days of antibiotics.
- If it’s gone, start of pulse therapy: 5 days of high-dose corticosteroids to control lung inflammation.
Pulse therapy can’t be done with the presence of bacteria because it deactivates the entire immune system.
So we’re praying that this nasty bug has been beaten up by the antibiotics.
Then, they’ll see how he reacts and adapt the following treatment.
The stressful points of our daily life (we need to talk about it)
Tonight, they lowered the oxygen concentration of Gabriel’s machine to 35%, which seems to be a good thing (the goal being 21%). But when I asked why, the doctor told me that excess oxygen could damage the lungs. However, another doctor, who had set it to 60%, had told me that oxygen was like a medicine.
The kind of contradiction that doesn’t help reduce stress…
Finally, for several days, I’ve noticed that some of the staff (usually the youngest or those who seem to be beginners) give the impression of being afraid to take care of Gabriel. And for us, as parents, it’s obviously very worrying.
From what I’ve observed and by asking a few questions, I have the impression that this fear comes from the fact that Gabriel reacts very strongly to each manipulation: diaper change, position change, or even physiotherapy session. Each time, he starts crying, holds his breath, his heart races, and he turns all red.
For us, it’s distressing, and I imagine that for someone who’s just starting, this kind of reaction is very impressive, even destabilizing. And sometimes we have the impression that they don’t dare take care of him for fear of provoking these episodes.
This situation also generates stress on our side. Because we wonder if he’s really receiving all the care he needs, or if some are avoided or postponed for fear of doing wrong…
Gabriel Was Baptized
Today, a very special moment took place for Gabriel.
On the advice of a friend, Manuela organized a baptism at the hospital, with the help of social workers and the psychologist.
The idea was to bring additional spiritual support to our little warrior, hoping that it could help in his healing.
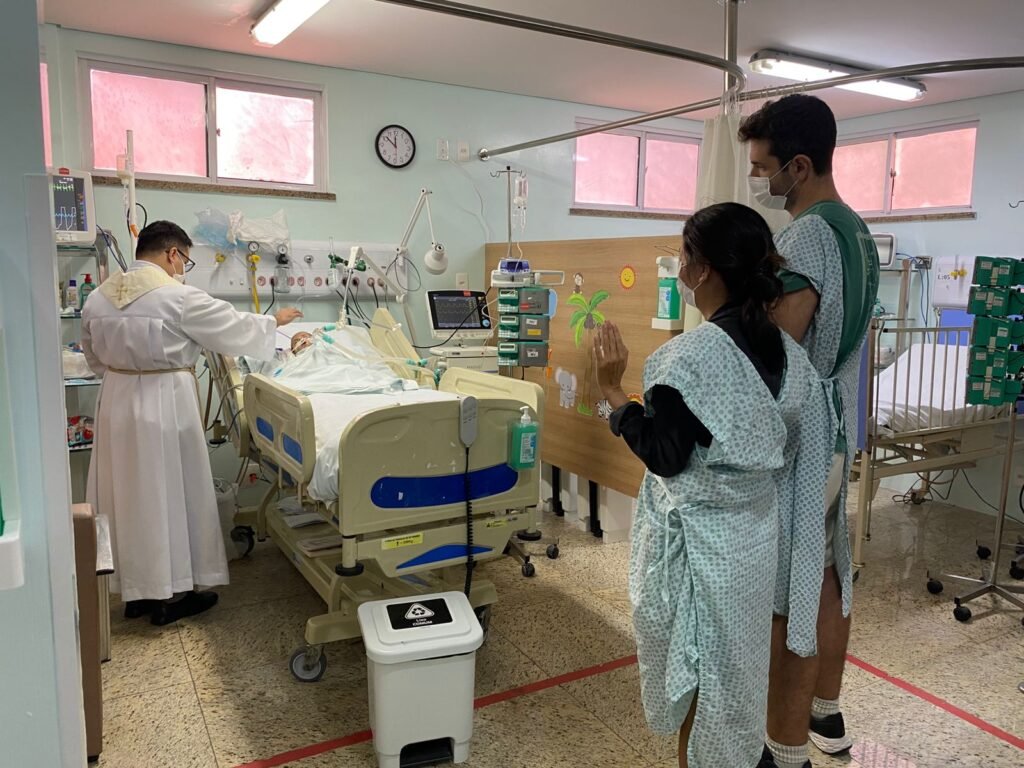
At noon, Father Tiago came to the ICU to celebrate what’s called an ’emergency baptism’.
We were just in front of his bed with the priest, and behind us, all the staff of the unit had gathered in a semicircle around Gabriel.
It was a deeply moving moment.
A more complete ceremony will take place later, with the godmothers and godfathers, when Gabriel leaves the hospital.
I’m also including a photo from the moment, which allows you to understand the conditions we’ve been living in every day for 6 weeks. Because in theory, photos are forbidden in the intensive care unit, but here the staff sent us some photos.
Life at the Hospital
These last few days, life at the hospital has been more lively.
Efforts are clearly underway to improve hygiene and reception, both for patients and parents.
Today, a manager from the hygiene department contacted me to gather my feedback on areas for improvement. So I shared a list of what I had already reported since our arrival. Some things have already changed for the better, and it’s important to acknowledge that.
This afternoon they went fly hunting, for example.
New developments in the waiting room next to the intensive care units
I sometimes think the hospital is disconnected from the reality families experience in the ICU.
They seem to want to encourage parents to stay as long as possible with their child, whenever the intensive care unit is open. But they don’t seem to realize how challenging this presence is.
Staying for hours next to your intubated child, connected to constantly beeping machines, with tubes everywhere, while hearing or seeing other children in sometimes critical situations… it’s a gut-wrenching experience. Personally, and I think this is the case for many parents here, I sometimes can’t manage to stay for more than twenty or thirty minutes at a time. Not for lack of love or will, but because it’s emotionally and physically exhausting.
And to that, you have to add an uncomfortable chair, with no possibility to lie down, even for a few minutes. We try to rest, but we end up with a twisted neck and an aching back.
So yes, the teams want us to stay with our child, but when we leave, we’re often drained because we’ve given everything not to break down in front of them.
Before, in these moments, we could go and lie down for a few moments on a sofa bed in the waiting room.
It was a small respite, a moment to breathe and regain strength before returning to the room.
Today, these sofas have been removed and replaced with hard, uncomfortable chairs, with the idea, it seems, of preventing parents from sleeping on site and encouraging them to go home.
Frankly, in my opinion, this is neither realistic nor humane.
The intention was to avoid the accumulation of people in the waiting room, but I think it’s not a good idea.
Many parents have even already mentioned the “idea of” bringing a mattress to sleep on the floor. Not sure we’re gaining in hygiene…
Rather than preventing families from resting, they should instead offer them a suitable, dignified, and soothing space but with hygiene standards to be respected.
Because accompanying a child in the ICU is not just “staying beside them”, it’s surviving, every day, an immense psychological ordeal!
Conclusion
As you can see, this day has been, once again, very emotionally charged.
My intention is simply to share, as close to reality as possible, what we experience on a daily basis.
I am in no way trying to criticize the hospital or its staff.
And in fact, quite the contrary: the ICU is undoubtedly the most competent department in the entire hospital, both in terms of medical expertise and support. And the administration is truly attentive.
What we want is for everything to continue to progress, for Gabriel to fully recover, and for us to be able to quickly return to a normal life.
